Crisis & Disaster Preparedness Guide for People with Diabetes
Mohammad Khalifah, Diabetes Educator, Imperial College London Diabetes & Endocrine Centre
Emergencies can limit access to insulin, medications, food, clean water, or electricity. Stress, lack of supplies, and interrupted routines can make diabetes management difficult and dangerous [1][2].
Being prepared protects your health and can save your life.
1. Why Preparation Matters
Disasters natural or human made can damage healthcare systems, cut off medication access, disrupt food and water supplies, and increase stress. This often leads to worsening blood glucose and higher risk of complications like DKA or severe hyperglycemia [2][3].
People with type 1 diabetes are especially vulnerable because they cannot survive without insulin [4].
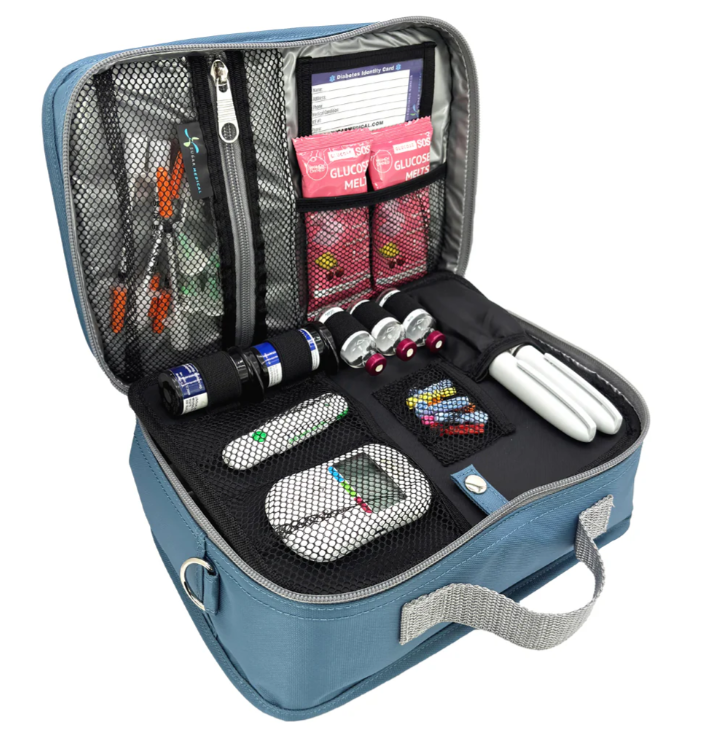
2. Your Diabetes Crisis Kit (Pack in an easy to carry bag)
A. Medicines & Insulin Supplies
- Insulin for 1–2 weeks, including long acting and rapid acting insulin [1].
- Spare insulin pens, syringes, or pump backup supplies [1].
- Pump infusion sets or pods for at least one week [1].
- CGM sensors or enough glucose strips for 100–150 checks [1].
- Glucagon emergency kit if available [5].
B. Monitoring Equipment
- Glucose meter with extra batteries [1].
- Lancets and lancing device.
- Urine or blood ketone strips (important for detecting DKA risk) [1].
C. Low Blood Sugar Treatment
- Glucose tablets
- Juice boxes or sweets
- Honey packets
- Long acting snacks like crackers or dates
D. Insulin Storage & Cooling
- Insulated pouch or cooling wallet
- Ice packs (wrap them; do not freeze insulin)
- Keep insulin protected from high temperature or freezing, which reduces effectiveness [6].
E. Important Documents
- Copy of ID
- List of all medications and doses
- Emergency contacts
- Written pump settings: basal rates, carb ratio, correction factor [1]

F. Food & Water
- Bottled water
- Ready to eat foods (nuts, canned food, protein bars,dates)
- ORS/electrolyte packets
G. Hygiene Items
- Alcohol wipes
- Hand sanitizer
- Bandages
- Safe sharps disposal container
3. What To Do in Emergency Situations
A. Power Cuts
- Keep insulin cool in insulated pouches.
- Avoid opening the refrigerator often.
- Switch to your glucose meter if your CGM or phone runs out of battery.
- If insulin is stored above recommended temperature, monitor sugars more closely until conditions improve [6].
B. Natural Disasters (Storms, Floods, Fires)
- Keep your kit with you at all times.
- Drink clean water regularly.
- Shelters may have limited healthy food choices and medication access, which can worsen blood sugar control [2].
- Check glucose frequently and treat highs/lows promptly.
C. Wars, Conflict, and Displacement
People with diabetes; especially insulin users, are extremely high-risk during war due to lack of insulin access, displacement, trauma, and food or water shortages [4].
During conflict:
- Keep your crisis kit always ready.
- Carry fast acting carbs in your pocket in case of lows.
- Store insulin in the coolest possible safe location.
- Wear visible medical ID.
- Inform relief workers immediately that you require insulin and glucose monitoring.
- Humanitarian laws protect the medical needs of civilians, including access to insulin and supplies [4].
D. Illness, Fever, Infection (Sick Day Rules)
Illness raises blood glucose and increases the risk of DKA or dehydration [7].
Follow these rules:
- Never stop your long acting insulin and always take your short acting insulin based on carbohydrate intake and your correction factor [7].
- Assess if any insulin doses were missed in the last 24 hours.
- If a long‑acting insulin dose was missed, take your usual long‑acting insulin.
- If a short‑acting dose was missed, take your usual rapid‑acting insulin.
- Check your glucose every 2-4 hours [7].
- Maintain good hydration; drink small amounts of fluids regularly to stay hydrated, ( IV fluids may be needed if dehydrated).
- Check ketones if your glucose is >250 mg/dL (13.9 mmol/L) or if you feel unwell [7].
- Check Blood ketones using ketone meter.
- >3mmol/l : seek medical help immediately
- 1.6 to 2.9mmol/l: High risk to progress to DKA, Take missed dose of insulin and ensure adequate hydration
- 0.6 to 1.5mmol/l: Take missed dose of insulin and ensure adequate hydration
- Re-check ketones every hour until they are below 0.6 mmol/L.
- If ketones remain above 0.6 mmol/L, seek medical care immediately.
- If you are vomiting, unable to keep fluids down, or ketones are high, seek urgent medical help.
4. Special Instructions for Type 1 Diabetes (T1DM)
People with type 1 diabetes need insulin every day for survival. During disasters, blood glucose usually becomes harder to control, and the risk of DKA rises significantly [2].
- Always keep long-acting insulin as a backup, even if you use a pump.
- If pump fails, switch to long-acting insulin immediately.
- Check ketones every 4 hours when sick or when glucose is high.
- Keep glucagon available.
- Drink fluids frequently.
- War and conflict conditions greatly increase danger; lack of insulin can cause life‑threatening DKA within days or even hours [4].
5. Special Instructions for Type 2 Diabetes Using Insulin (T2DM)
- Continue basal insulin even if you are not eating.
- Drink plenty of fluids.
- Check glucose every 4–6 hours.
- If you use SGLT2 inhibitors (e.g., Forxiga, Jardiance), STOP them during illness to reduce risk of ketoacidosis.
- Treat lows using the 15‑15 rule: 15g fast carbs, wait 15 minutes, recheck [8].

6. Quick Emergency Steps
Low Blood Sugar (<70 mg/dL / 3.9 mmol/L)
(15–15 Rule) [8]
- Take 15 g fast carbs
- Wait 15 minutes
- Re-check glucose
- Repeat if still low
High Blood Sugar (>250 mg/dL / 13.9 mmol/L)
- Check ketones
- Drink water
- Take correction insulin
- Seek medical help if ketones moderate/high or vomiting [7]
7. When to Seek Emergency Care
Seek urgent help if:
- You cannot access insulin
- You have high ketones
- You are vomiting or dehydrated
- Your glucose stays very high despite insulin
- You have symptoms of DKA (nausea, vomiting, fruity breath, fast breathing) [7]
References
1. American Diabetes Association. (n.d.). Tips for Emergency Preparedness. https://diabetes.org/tools-resources/disaster-relief/tips-for-emergency-preparedness [diabetes.org]
2. Johns Hopkins Diabetes Guide. (2016). Disaster Emergency Preparedness in Diabetes. Disaster Emergency Preparedness in Diabetes | Johns Hopkins Diabetes Guide
3. Centers for Disease Control and Prevention. (2024). Diabetes Care During Emergencies. https://www.cdc.gov/diabetes/articles/diabetes-care-emergencies.html [cdc.gov]
4. Jenkins, A. J., et al. (2024). People who need insulin are particularly vulnerable in disasters and conflicts. BMJ, 385, q1109. https://www.bmj.com/content/bmj/385/bmj.q1109.full.pdf [bmj.com]
5. Diabetes Disaster Response Coalition. (n.d.). Preparedness Resources. https://diabetesdisasterresponse.org/ [diabetesdi...sponse.org]
6. Centers for Disease Control and Prevention. (2024). Managing Insulin in an Emergency. https://www.cdc.gov/diabetes/articles/managing-insulin-in-emergency.html [cdc.gov]
7. American Diabetes Association. (n.d.). Planning for Sick Days. https://diabetes.org/getting-sick-with-diabetes/sick-days [diabetes.org]
8. Diabetes Emergency Resources (DEFA). (2023). The 15‑15 Rule for Treating Low Blood Glucose. https://www.diabetesdefa.org/collection/disaster-response-resources-ddrc [diabetesdefa.org]






